For Professionals Who Care Deeply
You’re doing everything you can. But you can’t do it all.
As a pediatrician, therapist, or school provider, you care deeply about your families — but feeding concerns? They’re messy, complex, and time-consuming.
You’ve probably been there:
A child eats five foods… but they’re still growing
A parent insists something is wrong… but you don’t see a clear medical diagnosis
You want to help… but you’re out of time, tools, or referrals
That’s where a trusted feeding therapy referral makes all the difference.
You want to support them. But you also don’t have 45 minutes to explain sensory feeding aversions, oral motor delays, or ARFID.
That’s where Foodology Feeding steps in.
What Happens After You Refer a Family
A structured pathway designed to uncover the root cause of feeding struggles and create meaningful progress for families.
Comprehensive Evaluation
We evaluate oral-motor function, sensory processing, nutritional patterns, medical history, and mealtime dynamics. When clinically appropriate, families also complete food sensitivity testing and a stool gut sample to assess microbiome health, permeability, and underlying contributors.
Targeted Implementation
Families move directly into an initial package that includes 8 implementation sessions, so they are never left trying to figure out what to do after the evaluation. This phase turns findings into guided, practical progress through parent coaching and clear next steps.
Ongoing Support When Needed
For more complex cases, families may continue with twice-monthly 45-minute support sessions. When direct oral-motor work with the child is needed, we include the child on calls as appropriate to support progress more directly.
Help Families Access Insurance Coverage
We provide physicians with a simple documentation template that can help support medical necessity when families pursue out-of-network reimbursement or a gap exception for feeding therapy.
Download Medical Necessity TemplateProviders may modify this template as needed based on clinical judgment and patient diagnosis.
For families you believe may benefit from a deeper feeding evaluation.
Questions About a Case?
Our clinical team is happy to help determine whether a feeding evaluation may be appropriate.

References for Feeding Statistics & Nutritional Impact
¹ Taylor, C. M., Wernimont, S. M., Northstone, K., & Emmett, P. M. (2015).
Picky/fussy eating in children: review of definitions, assessment, prevalence and dietary intakes. Appetite, 95, 349–359.
https://doi.org/10.1016/j.appet.2015.07.026
² Thomas, J. J., Lawson, E. A., Micali, N., Misra, M., Deckersbach, T., & Eddy, K. T. (2017).
Avoidant/restrictive food intake disorder: a three-dimensional model of neurobiology with implications for etiology and treatment. Current Psychiatry Reports, 19(8), 54.
https://doi.org/10.1007/s11920-017-0800-0
³ Goday, P. S., Huh, S. Y., Silverman, A., Lukens, C. T., Dodrill, P., Cohen, S. S., Delaney, A. L., Feuling, M. B., Noel, R. J., Gisel, E., Kenzer, A., & Browne, J. V. (2019).
Pediatric Feeding Disorder: Consensus Definition and Conceptual Framework. Journal of Pediatric Gastroenterology and Nutrition, 68(1), 124–129.
https://doi.org/10.1097/MPG.0000000000002188
⁴ Dovey, T. M., Staples, P. A., Gibson, E. L., & Halford, J. C. G. (2008).
Food neophobia and ‘picky/fussy’ eating in children: A review. Appetite, 50(2–3), 181–193.
https://doi.org/10.1016/j.appet.2007.09.009
⁵ Rucklidge, J. J., Johnstone, J., & Kaplan, B. J. (2014).
Nutrition and mental health: mainstreaming dietary treatment in clinical practice. The Lancet Psychiatry, 1(5), 400–402.
https://doi.org/10.1016/S2215-0366(14)70344-1
⁶ Kennedy, D. O. (2016).
B Vitamins and the Brain: Mechanisms, Dose and Efficacy—A Review. Nutrients, 8(2), 68.
https://doi.org/10.3390/nu8020068
We Make You the Hero
(Without Extra Work)
We’re a specialized feeding therapy team that helps families get real answers and tangible progress — while making you look like the provider who connected the dots.
When you refer to Foodology, here’s what you can expect:
✅ A thorough evaluation and action plan parents have been begging for
🕒 Progress updates (with consent) — no extra admin for you
💬 No pressure to “diagnose” outside your scope
🙌 Confidence that tricky cases are being handled seriously and holistically
And the best part?
You won’t see that same family cycling through your office again and again with no plan.
You Get to Be the Provider Who Listened
The one who didn’t dismiss a parent’s gut feeling.
The one who offered real help.
The one who referred them to someone who could finally make a difference.
Let us take those “problem feeders” off your hands — and give you peace of mind that they’re getting the support they need.
Your Role Is Incredibly Valuable
Your referral might be the moment that changes everything.
We’ll handle the rest — thoroughly, respectfully, and with a holistic lens.
👇 Keep reading to see how we approach feeding — and when to refer.
Clinical Indicators for Feeding Therapy Referral
Children
If you’re unsure whether feeding therapy is warranted — these are the cases we specialize in.
Even when children are “growing fine,” the red flags below may indicate a deeper issue.
Refer if a child:
Eats fewer than 20 total foods
Eliminates entire food groups or textures
Refuses previously accepted foods (and doesn’t regain them)
Gags, vomits, or cries in response to food exposure
Insists foods be prepared exactly the same way
Shows extreme rigidity, anxiety, or panic at meals
Has ongoing constipation, reflux, or suspected food sensitivities
Is stuck at a feeding milestone (e.g., never progressed from purées)
Avoids eating in front of others or at school
Experiences distress when asked to try or even be near new foods
Infants
Feeding challenges start early — and they’re often missed or misdiagnosed.
We offer expert evaluations for infants with:
Difficulty latching or staying on the breast/bottle
Excessive spit-up, arching, or gas
Poor weight gain or feeding fatigue
Suspected tongue or lip ties
Transition issues to solids
We assess oral-motor function, guide families through feeding techniques, and provide referrals when bodywork is also needed.
Early feeding concerns don’t always go away on their own. A referral today can prevent bigger challenges later.

Checklists and Tools for Pediatricians
ARFID/PFD
Spot the red flags. Know what’s normal. Refer with confidence.
Feeding issues are often dismissed or misclassified as “just picky eating.” But if left unaddressed, they can spiral into nutritional deficiencies, anxiety, ARFID, or Pediatric Feeding Disorder (PFD).
That’s why we created this simple, therapist-designed checklist — to help you:
✅ Identify when picky eating is no longer typical
✅ Understand which behaviors warrant referral
✅ Support parents without jumping to judgment or false reassurance
✅ Save time in appointments by having a clear decision-making tool
INFANTS
Catch feeding concerns before they spiral — even in babies.
Feeding difficulties can start long before solids — from latch issues to silent reflux to bottle refusal. And too often, infant struggles are dismissed as “normal” or blamed on parental anxiety.
Our Red Flags Brochure for Infants gives you a quick guide to:
✅ Recognize early signs of feeding dysfunction in babies
✅ Know when tongue tie, reflux, or bottle refusal may warrant referral
✅ Empower parents without adding pressure
✅ Avoid the “wait and see” trap that delays care
Designed to support faster decision-making at well visits — and help you refer with confidence, even in those tricky under-12-month cases.

📦 Want printed copies for your office? Just let us know — we’ll send them.
“This is exactly what I needed — clear, concise, and based on real feeding therapy experience. I keep it in my drawer for every 18-month and 2-year well check.”
— Pediatrician in Long Island, NY

Feeding Disorders at a Glance
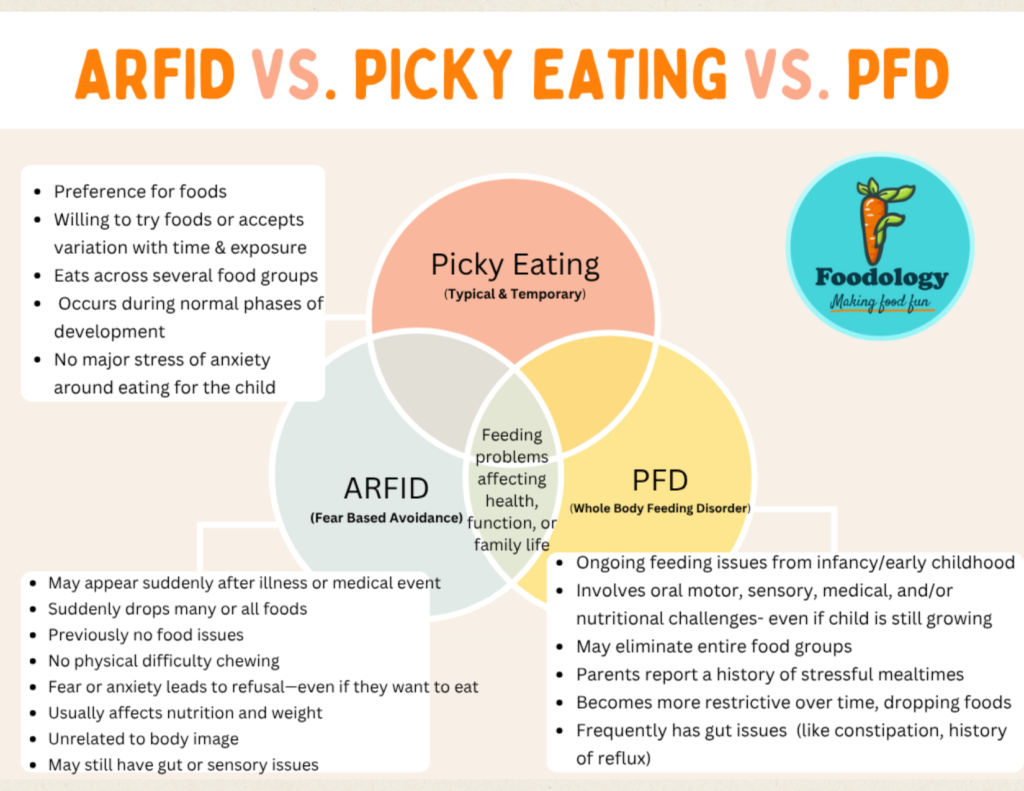
PFD, ARFID, or Just Picky?
Not all selective eating is the same — and not every child will grow out of it.
This diagram breaks down the key differences between developmental picky eating, ARFID, and Pediatric Feeding Disorder — so you can make informed referrals with confidence.


Infant Feeding: What’s Normal — and What’s Not?
Feeding challenges in infancy often go unrecognized — but early red flags can signal deeper issues.
This resource outlines the most common signs of infant feeding difficulty, including oral-motor concerns, reflux-like behavior, and delayed transitions to solids.
Know what’s typical… and when to refer.
Our Approach: The 4 Pillars of Feeding Success™
We don’t just manage symptoms. We get to the root.
At Foodology, we specialize in complex feeding cases by addressing the true source of mealtime struggles — not just the surface behaviors.
Our proprietary framework, The 4 Pillars of Feeding Success™, guides every evaluation and intervention.
1. Oral-Motor Function
Subtle deficits can severely impact chewing, swallowing, or food variety — especially when structural issues (like tongue tie or jaw instability) go undetected.
➡️ We assess chewing patterns, bolus formation, postural stability, and oral coordination to uncover what others often miss.
2. Sensory Processing
Over- and under-responsivity across the 8 sensory systems — especially tactile, gustatory, and interoception — can drive refusal, anxiety, or avoidance.
➡️ We use sensory-informed strategies to match the child’s regulation profile and build food tolerance without pressure.
3. Gut & Nutritional Health
Constipation, food intolerances, histamine overload, and nutrient gaps all affect appetite, regulation, and mealtime success.
➡️ We collaborate with functional providers and use evidence-based strategies to support gut–brain balance and reduce internal distress.
4. Feeding Mindset & Nervous System Regulation
Feeding is relational. Trauma, anxiety, and nervous system dysregulation disrupt safety, trust, and curiosity around food.
➡️ We integrate co-regulation techniques, play-based exposure, and our signature subliminal audio tools to support rewiring at the subconscious level.
Together, these pillars allow us to differentiate between:
🟡 Developmental picky eating
🔴 ARFID (Avoidant/Restrictive Food Intake Disorder)
🟣 Pediatric Feeding Disorder (PFD)
✅ This whole-child lens is what sets us apart — and why we often see progress when traditional therapy has failed.
🌍 Available Worldwide
Whether you’re in New York or New Zealand, we offer virtual services for families across the globe — including evaluations, parent coaching, and online programs.
Testimonials
“We spent a year in feeding therapy with no results.”
“Nothing clicked until we worked with Christine. This program explained things no one ever had — and it actually worked. I wish we had started here first.”
— Sarah, mom of a 5-year-old in the Fearful™ stage
“The only feeding referral I trust to get results.”
“I’ve referred multiple families to Foodology and every single one came back saying they finally felt heard. The reports are clear, actionable, and respectful of our role as providers.”
— Pediatrician, Long Island, NY
Frequently Asked Questions
Do I need to diagnose ARFID or PFD before referring?
Not at all.
We handle the evaluation and differential process. Many children don’t fit neatly into a diagnosis — that’s where our whole-child approach shines. You simply refer based on concern.
Do you take insurance?
We Fill the Gap That Insurance-Based Clinics Often Miss
Unlike most insurance-based therapy providers, we don’t just check a box or follow a 6-session template.
We specialize in complex, layered feeding cases — the ones that often get dismissed, delayed, or underserved in traditional systems.
That’s why we’re private-pay only — so we can provide the depth of evaluation, individualized planning, and ongoing support these families truly need.
But we also know cost matters.
We offer tools to help families access out-of-network reimbursement:
A downloadable Insurance Appeal Toolkit with ready-to-use templates and parent guides
Customized superbills that reflect medically necessary services and align with insurer language
Can families use HSA or FSA funds?
Yes — most of our services are eligible for HSA/FSA payment. We also provide detailed receipts and documentation to support that process.
Can you work with families outside New York?
Absolutely.
We provide virtual evaluations, coaching, and courses worldwide — helping families across the U.S. and internationally. Feeding issues don’t stop at state lines, and neither do we.
What happens after I refer a family?
Once the family contacts us, we begin with a thorough intake to understand the child’s feeding history, current challenges, and family goals.
We then guide them through the next best step — which may include:
A virtual or in-person evaluation based on location, severity, and support needs
A detailed assessment of oral-motor, sensory, nutritional, and behavioral components
A personalized Roadmap or plan of care that outlines how we will address root causes of feeding challenges
With parent consent, we’ll send you a summary of findings and next steps.
You’ll also receive brief, relevant updates — so you stay informed without additional paperwork or time taken from your day.
Our goal is to give your families the comprehensive support they need — and give you peace of mind that they’re in expert hands.
What kinds of cases are a good fit for Foodology?
We specialize in:
Children who eat fewer than 20 foods
- Infants with feeding difficulties (e.g., latch issues, poor transfer, oral motor concerns, poor weight gain, mom struggling to breasstfeed)
Kids with oral-motor delays, sensory sensitivities, or anxiety around eating
Families who’ve tried traditional therapy with little progress
Suspected ARFID or PFD
Parents who feel dismissed or desperate for answers
See other free resources

Refer parents to How to Un-Picky Your Picky Eater — a podcast hosted by Christine Miroddi Yoder, pediatric feeding expert and founder of Foodology. Each episode offers practical, holistic tips to help parents reduce mealtime stress and support their child’s relationship with food.

Our blog covers evidence-informed insights into Pediatric Feeding Disorder, ARFID, and picky eating.
Explore practical articles you can share with parents or use to guide conversations during well visits and therapy sessions.